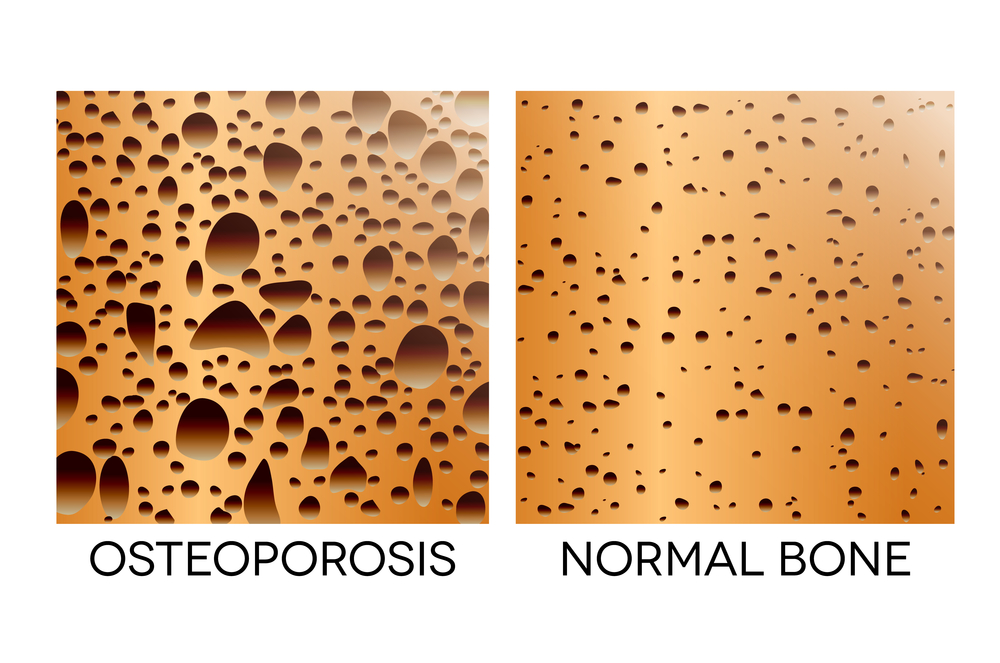
To treat osteoporosis, you need to focus on both preventing fractures and strengthening bones with medication.
Although a diagnosis of osteoporosis is based on the results of your bone density scan, the decision about what treatment you need, if any, is based on a number of other factors including your:
- age
- sex
- risk of breaking a bone
- previous injury history
Even if you have been diagnosed with osteoporosis because you have had a broken bone, you should still receive treatment to reduce your risk of further broken bones.
You might not require or want to take medication to battle osteoporosis. You should make sure you’re getting enough calcium and vitamin D. To make sure you’re getting the right nutrients, your healthcare team will ask you about your diet and may recommend changes or supplements.
Medicines for Osteoporosis
A number of different medicines are used to treat osteoporosis (and sometimes osteopenia).
1. Bisphosphonates
Bisphosphonates are drugs used to treat osteoporosis. They work by slowing the rate at which bone is broken down in your body. This helps to keep your bones strong and less likely to break. There are a number of different bisphosphonates, including:
- alendronic acid
- ibandronic acid
- risedronate
- zoledronic acid
You should always take bisphosphonates on an empty stomach with a full glass of water. After taking them, stand or sit upright for 30 minutes. After you have your blood drawn, you will need to wait 30 minutes to 2 hours before consuming any food or fluids.
The effects of bisphosphonates typically take 6 to 12 months to manifest, and patients may need to take the medication for 5 years or more. You may also be prescribed calcium and vitamin D supplements to take separately from the bisphosphonate.
The main side effects associated with bisphosphonates include:
- irritation to the food pipe
- swallowing problems
- stomach pain
Osteonecrosis of the jaw is a rare side effect linked with the use of bisphosphonates. Most cases occur with high-dose intravenous bisphosphonate treatment for cancer, rather than for osteoporosis.
In osteonecrosis, the cells in the jaw bone die due to a lack of blood supply, which can lead to problems with healing. If you have had dental problems in the past, you will need to have a check-up before you start treatment with bisphosphonates. Speak to your doctor if you have any concerns.
2. Selective Estrogen Receptor Modulators (SERMs)
SERMs are medicines that have a similar effect on bone as the hormone estrogen, but they are not as powerful. They help keep bones strong and decrease the chance of breaking them, especially in the spine area.
There is only one type of SERM (selective estrogen receptor modulator) that can be used to treat osteoporosis, and that is raloxifene. It’s only recommended for women, after menopause. It’s taken as a daily tablet. Side effects associated with raloxifene include:
- hot flushes
- leg cramps
- a potential increased risk of blood clots
3. Parathyroid Hormone
Parathyroid hormone is produced naturally in the body. It regulates the amount of calcium in bone. Treatments that stimulate the cells that create new bone, such as parathyroid hormone treatments (such as teriparatide), are used to manage conditions related to bone loss. You take them as an injection once a day.
Although other medications can reduce the rate at which bones degrade, parathyroid hormone can actually increase bone density. The medication is only effective for a small number of people with very low bone density. It is only used when other treatments have failed.
The treatment may cause nausea, headaches and dizziness.
4. Biological Medicines
Biological medicines are made from proteins or other substances produced by the body, as opposed to being created synthetically.
There are two types of biological medicines that can be used to treat osteoporosis: denosumab and romosozumab. If you cannot take other medicines for osteoporosis, such as bisphosphonates, denosumab may be a good option.
They slow the rate of bone breakdown and speed up the rate at which cells build bone. Injections are given either monthly or every few months. The most common side effects are muscle or joint pain, rashes, constipation, and cold-like symptoms.
5. Calcium and Vitamin D Supplements
If you want healthy bones, you need to have enough calcium in your diet. Calcium is the main mineral found in bone.
The recommended amount of calcium for most healthy adults is 700 milligrams (mg) a day. This can usually be obtained through a varied diet that contains good sources of calcium.
If you are diagnosed with osteoporosis, you will likely need to increase your calcium intake through supplements. Ask your GP for advice about taking calcium supplements.
Vitamin D helps the body absorb calcium. Doctors recommend that all adults should consume 10 micrograms of vitamin D on a daily basis. From March to September, people can get vitamin D from sunlight.
Pregnant and breastfeeding women should take a daily supplement of 10 micrograms of vitamin D during the autumn and winter.
6. Boron
Boron is not an essential nutrient, meaning you don’t need it in large amounts for your body to function. This is important because it allows your body to use calcium effectively. In addition, boron helps to treat osteoporosis by activating vitamins and minerals needed for strong bones.
You will need to take between 3 and 5 mg of boron each day in order to help treat your osteoporosis. This substance is present in foods such as apples, grapes, nuts, peaches, and pears.
Boron isn’t commonly found in multivitamins. Consult with your physician to see if taking a boron supplement would be advantageous for you. If you take a multivitamin, be aware of potential side effects from taking too much, such as feeling nauseous, vomiting, tired, and having diarrhea.
7. Magnesium
The body doesn’t store magnesium. The body needs a regular intake of magnesium from foods and/or supplements to maintain healthy levels, as it is a mineral naturally found in foods like whole-grain breads, dark green vegetables, and nuts. Magnesium and calcium are essential for strong bones. They work together to keep bones healthy and prevent breaks.
You should aim to consume between 300 and 500 mg of magnesium every day. If you eat a lot of processed foods, it’s likely that you’re not getting enough magnesium in your daily diet.
Magnesium can be obtained through supplements, but it is often found in daily multivitamins. An ideal balance is two calcium atoms for every one magnesium atom. A multivitamin with 1,000 mg of calcium should have 500 mg of magnesium.
Be on the lookout for indications that you are getting too much magnesium, like an upset stomach or diarrhea. These symptoms indicate you should cut back on magnesium.
8. HRT (Hormone Replacement Therapy)
Menopause is a time when a woman’s periods stop. Hormone Replacement Therapy (HRT) can be taken to help control symptoms associated with the menopause.
HRT has also been shown to improve bone density and reduce the risk of developing osteoporosis. If you already have osteoporosis, taking medication can help to improve your condition by strengthening your bones and reducing your risk of fracturing them.
If you experience early menopause, your doctor will likely advise you to take HRT or a hormonal contraceptive until you are at least 51 years old. If you have a high level of estrogen, you are less likely to get osteoporosis or other health conditions.
HRT slightly increases the risk of breast cancer. The longer you take HRT, the higher your risk will be. HRT in tablet form has a slightly higher risk of causing blood clots than other forms such as patches, gel, or spray.
The decision of whether or not to take HRT depends on various factors such as your age, the severity of your symptoms, and any possible risks involved. If you’re experiencing menopause symptoms and you’re 60 years old or younger, the benefits of HRT will usually be greater than the risks.
9. Herbal Supplements
Not all women can or want to take hormone treatments for osteoporosis. Alternative treatments include Chinese herbs and other supplements. Many of the treatments for conditions like bipolar disorder and depression are not backed by extensive research, so their potential side effects are not well known.
A 2013 review of studies published in the Journal of Traditional and Complementary Medicine found that a combination of three herbs was studied for its effect on postmenopausal women. The herbs – Herba epimedii, Fructus ligustri lucidi, and Fructus psoraleae – were given in a ratio of 10:8:2.
The ELP formula was found to have bone-protective effects in postmenopausal women. The herbs used are reported to have estrogen-like effects.
Alternative Treatments
There are other herbs that may help with treating osteoporosis, such as black cohosh and horsetail. There is not much research on how these two herbs impact osteoporosis.
The goal of any alternative treatment is to manage or heal the condition without having to rely on medication. Some alternative therapies can be used for osteoporosis. Although there is little scientific proof that they are effective, many people say that they have had success.
Red clover is thought to contain estrogen-like compounds. Some alternative care practitioners may recommend the use of natural estrogen to treat osteoporosis because it can help protect bone.
Although there is no scientific evidence, some people believe that red clover can help to slow down bone loss.
The estrogen-like properties of red clover may interact with other medications, and may not be a good fit for everyone. Before taking red clover, be sure to speak with your doctor. There are significant possible drug interactions and side effects.
Isoflavones are found in soybeans and are used to make products like tofu and soy milk. Isoflavones are tell your body to produce less bone-thinning compounds and to stop bone loss.
Soy is often recommended for osteoporosis, but it’s important to speak to a doctor first, especially if you’re at a higher risk for estrogen-dependent breast cancer.
Native Americans have used black cohosh as medicine for many years. It also has been used as an insect repellant. The plant contains substances known as phytoestrogens, which are similar to the hormone estrogen. These substances may help to prevent bone loss.
A 2008 study found that black cohosh had positive effects on bone formation in mice. To determine if these results can be extended to treatment in humans with osteoporosis, more scientific research is needed.
Talk to your doctor before taking black cohosh, as it may have side effects.
Horsetail is a plant with possible medicinal properties. Horsetail is believed to help with bone loss by stimulating bone regeneration. One of the main active ingredients in horsetail is silicon.
Although there is a lack of clinical trials to support this assertion, some holistic doctors still recommend horsetail as an osteoporosis treatment.
Horsetail can be taken in many forms such as a tea, tincture, or herbal compress. When using this medication, it is important to stay properly hydrated and avoid alcohol, nicotine patches, and diuretics, as they can interact negatively with the medication.
Acupuncture is a therapy used in traditional Chinese medicine. The thin needles are placed in strategic points on the body. The method is thought to help different organs and body functions work better and to help the body heal.
Acupuncture is often combined with herbal therapies. There is some evidence to suggest that these two treatments may be effective in treating osteoporosis, but more research is needed to confirm this.
Tai Chi is the ancient Chinese practice that uses a series of body postures that flow smoothly and gently from one to the next.
The National Center for Complementary and Integrative Health has found that tai chi might help improve immunity and mental health in older adults.
Regular exercise may help to improve muscle strength, coordination, and reduce pain and stiffness in the muscles or joints. Regular, supervised exercise can help improve your balance and physical stability. It may also prevent falls.
The hormone melatonin is produced by the pineal gland in the human body. Melatonin has been praised for years as a natural sleep aid and an agent that reduces inflammation. There is a growing body of research that suggests that melatonin may promote healthy growth of bone cells.
Melatonin is a natural hormone that is available in capsule, tablet, and liquid form. It is considered safe to take. However, it can make you sleepy and can interfere with antidepressants, blood pressure medications, and beta-blockers, so you should speak to your doctor before taking it.
Treatment Conclusion
When someone is diagnosed with osteoporosis, they are told to change their diet to incorporate more calcium. Although you cannot instantly fix your bone mass, you may be able to prevent further bone loss by making dietary changes.
Hormone replacement drugs, particularly the ones containing estrogen, are generally prescribed. Hormone therapy drugs have side effects that may negatively impact other areas of your life.
Biophosphonate medications are commonly used to stop bone loss and reduce the risk of fractures. This class of medication may cause nausea and heartburn.
Some people with osteoporosis choose to try alternative methods because the synthetic medications used to treat it can have side effects. You should always talk to your doctor before taking any medication.
Prevention
Osteoporosis can be prevented. Physical activity helps to keep bones healthy. Lifting weights is a great way to exercise and maintain bone mass. Choosing to live a healthy lifestyle by not smoking and avoiding substance abuse can also help to reduce your risk of developing osteoporosis.
Vitamins that are good for your bones, like vitamin D, calcium, and vitamin K, should be a regular part of your diet to help avoid weak bones later on.