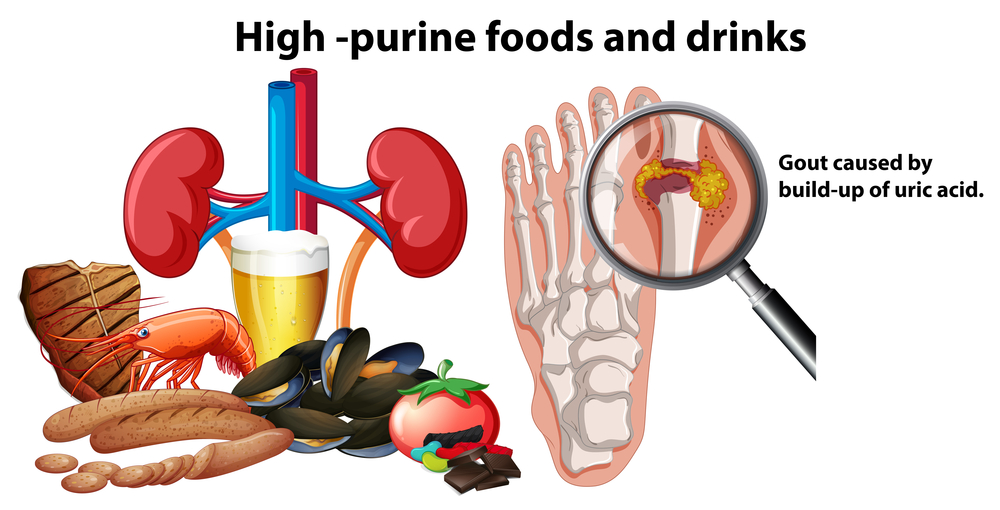
Gout is one of the most common forms of inflammatory arthritis—and also one of the most misunderstood. Many people think it’s simply caused by eating too much meat or drinking too much alcohol. While diet can play a role, gout is actually a complex condition that involves uric acid metabolism, kidney function, genetics, medications, and overall health. The good news is that gout is highly manageable. With the right treatment plan and a few practical lifestyle adjustments, many people can reduce flare-ups dramatically and protect their joints long-term.
In this article, you’ll learn what gout is, what triggers it, how it’s diagnosed, the most effective treatment options, and what to eat (and avoid) to prevent painful attacks.
What Is Gout?
Gout is a type of arthritis caused by the buildup of uric acid in the body. Uric acid is a natural waste product created when your body breaks down substances called purines. Purines are found naturally in your body and also in many foods.
Normally, uric acid dissolves in the blood, passes through the kidneys, and leaves the body in urine. But if your body makes too much uric acid—or your kidneys can’t remove enough of it—uric acid levels rise. When levels stay high, uric acid can form sharp, needle-like crystals in joints and surrounding tissues. These crystals trigger sudden inflammation, swelling, redness, and intense pain.
Gout often begins in the big toe, but it can affect ankles, knees, wrists, fingers, and elbows as well.
Common Symptoms of Gout
Gout symptoms tend to appear suddenly, often at night, and can feel severe. Typical signs include:
- Sudden, intense joint pain (often the big toe)
- Swelling and warmth in the affected joint
- Red, shiny skin over the joint
- Extreme tenderness—even a bedsheet touching the joint may hurt
- Limited range of motion during or after an attack
A gout attack may last several days to two weeks. Some people have one flare and then none for years, while others experience frequent flare-ups.
Chronic Gout and Tophi
If gout is not treated effectively over time, it can become chronic. Some people develop tophi—visible lumps of uric acid crystals that form under the skin, commonly around fingers, elbows, or ears. Chronic gout can also cause joint damage and deformity.
What Causes Gout?
Gout is driven by elevated uric acid, but multiple factors can contribute:
- Genetics
Family history strongly increases risk. If close relatives have gout, your odds are higher.
- Kidney Function
Kidneys that don’t clear uric acid well (even mildly reduced function) can lead to buildup.
- Diet (Purine-Heavy Foods)
Foods high in purines can increase uric acid, especially in people who are already predisposed. More on diet below.
- Alcohol and Sugary Drinks
Beer and spirits can raise uric acid and reduce how well the kidneys excrete it. Sugary drinks—especially those sweetened with fructose—can also spike uric acid.
- Weight and Metabolic Health
Obesity, insulin resistance, and metabolic syndrome are strongly associated with gout.
- Certain Medications
Some medications raise uric acid levels, including:
- Thiazide and loop diuretics (water pills)
- Low-dose aspirin
- Some immunosuppressants
- Dehydration and Rapid Weight Loss
Dehydration concentrates uric acid in the blood. Crash dieting or fasting can also trigger flare-ups.
Common Gout Triggers
Even when someone has high uric acid, attacks often follow a trigger such as:
- Heavy alcohol intake (especially beer)
- High-purine meals (organ meats, shellfish)
- Dehydration
- Illness, infection, or surgery
- Injury to a joint
- Sudden changes in diet (including very high-protein or “keto” shifts for some people)
Knowing your personal triggers can help you prevent future attacks.
How Gout Is Diagnosed
A healthcare professional may diagnose gout based on symptoms, exam, and tests such as:
- Blood test for uric acid (helpful, but levels can be normal during a flare)
- Joint fluid analysis (the most definitive test—looking for urate crystals)
- Ultrasound or dual-energy CT (DECT) in certain cases to detect crystal deposits
- X-rays to assess joint damage in chronic gout
If you suspect gout, don’t self-diagnose—other conditions like septic arthritis (joint infection) can look similar and require urgent care.
Gout Treatment: What Works Best
Treatment usually has two goals:
- Relieve pain and inflammation during attacks
- Prevent future attacks by lowering uric acid
Treating a Gout Flare (Acute Attack)
Common options include:
- NSAIDs (like ibuprofen or naproxen) if appropriate for you
- Colchicine, especially effective when taken early
- Corticosteroids (oral or injected) if NSAIDs aren’t safe
During a flare, rest the joint, elevate it, apply ice packs, and stay hydrated.
Preventing Gout Long-Term (Urate-Lowering Therapy)
If you have frequent flares, tophi, kidney stones, or joint damage, your clinician may recommend medications to reduce uric acid, such as:
- Allopurinol (commonly first-line)
- Febuxostat
- Probenecid (helps kidneys remove more uric acid in some cases)
Important note: starting urate-lowering therapy can temporarily increase flare risk at first, so clinicians often prescribe a short preventive course of colchicine or NSAIDs during the early phase.
Long-term management is about consistency. When uric acid is kept in a healthy range over time, crystal deposits shrink and flare-ups often become much less frequent.
The Best Diet for Gout: What to Eat and Avoid
Diet isn’t the only factor in gout, but it can help reduce flare frequency and improve overall health.
Foods to Limit or Avoid
These are commonly linked with higher uric acid or flare risk:
- Organ meats (liver, kidney)
- Certain seafood (anchovies, sardines, mussels, scallops)
- Red meat in large portions
- Alcohol, especially beer
- Sugary beverages (soda, sweetened juices, energy drinks)
- High-fructose corn syrup foods
Many people do well with a Mediterranean-style approach:
- Low-fat dairy (milk, yogurt) – often associated with lower uric acid
- Cherries and berries – may help reduce inflammation for some people
- Coffee (in moderation) – linked in some studies to lower gout risk
- Vegetables (including those with purines like spinach and mushrooms—these generally don’t trigger gout like meat does)
- Whole grains, beans, nuts, olive oil
- Water – hydration is a simple but powerful tool
Practical Eating Tips
- Focus on portion sizes rather than “never” foods.
- Build meals around vegetables + fiber + lean protein.
- Choose poultry, tofu, eggs, or legumes more often than red meat.
- Aim for steady, sustainable weight loss if needed—avoid crash diets.
When to See a Doctor
Seek medical care if:
- This is your first suspected gout attack
- The pain is severe or the joint is very swollen and hot
- You have fever (could indicate infection)
- You’re having frequent flares (more than 1–2 per year)
- You have kidney disease, kidney stones, or diabetes
Early diagnosis and proper treatment can prevent long-term joint damage.
Final Thoughts: You Can Control Gout
Gout can be incredibly painful, but it is also one of the most treatable forms of arthritis. The best outcomes come from a plan that combines flare treatment, uric-acid control when indicated, and lifestyle habits that reduce triggers. If you’re dealing with gout symptoms, talk with a healthcare professional—effective relief and long-term prevention are absolutely possible.
Sources:
https://www.mayoclinic.org/diseases-conditions/gout/symptoms-causes/syc-20372897
https://my.clevelandclinic.org/health/diseases/4755-gout
https://gouteducation.org/uric-acid/
Gout is one of the most painful forms of arthritis — and one of the most preventable. This ancient disease, caused by uric acid crystal buildup in your joints, affects millions of people. The good news? With the right treatment and dietary changes, gout is highly controllable.
What Is Gout?
Gout is a type of inflammatory arthritis that occurs when uric acid levels in your blood get too high. When your body can’t eliminate enough uric acid, it forms needle-like crystals that deposit in your joints, causing sudden and severe pain, swelling, and redness.
The condition typically affects one joint at a time — most commonly the big toe (called podagra) — but can also strike your ankle, knee, wrist, or elbow.
What Causes High Uric Acid?
Uric acid is a natural waste product your body creates when breaking down purines — substances found in your body’s cells and many foods. Normally, uric acid dissolves in your blood, passes through your kidneys, and leaves through your urine.
Gout develops when:
- Your body produces too much uric acid
- Your kidneys can’t eliminate enough of it (about 90% of cases)
- Or both
Gout Symptoms
Gout flares often start suddenly at night with:
- Intense joint pain — severe enough to wake you up
- Swelling and redness — the joint becomes warm and tender
- Limited mobility — moving the joint becomes difficult
- Systemic symptoms — fever, chills, and fatigue may accompany the attack
Flares typically last one to two weeks and then resolve. Without treatment, attacks may become more frequent and last longer over time.
Risk Factors for Gout
You’re more likely to develop gout if you:
- Are male (though women’s risk increases after menopause)
- Are middle-aged or older
- Have obesity
- Have high blood pressure, heart disease, or kidney disease
- Have a family history of gout
- Eat a diet high in purines (red meat, organ meats, certain seafood)
- Drink alcohol, especially beer
- Consume sugary drinks with high-fructose corn syrup
- Take certain medications (diuretics, low-dose aspirin)
Treatment Options
During a Flare
Treatment focuses on reducing pain and inflammation:
- NSAIDs — ibuprofen, naproxen, or indomethacin
- Colchicine — an anti-inflammatory that works best when taken early
- Corticosteroids — oral or injected when NSAIDs aren’t an option
Important: Don’t start uric acid-lowering medications during an active flare — it can actually make things worse.
Long-Term Prevention
To prevent future attacks:
- Allopurinol or febuxostat — xanthine oxidase inhibitors that reduce uric acid production
- Probenecid — increases uric acid excretion (not for those with kidney stones)
- Lifestyle changes — diet, weight loss, and limiting alcohol
The Gout Diet: What to Eat and Avoid
Foods to Limit or Avoid
- Red meat and organ meats — liver, kidney, sweetbreads
- Certain seafood — anchovies, sardines, mussels, scallops, trout
- Beer and liquor — alcohol slows uric acid excretion
- Sugary drinks — especially those with high-fructose corn syrup
- Ultra-processed foods — fast food and packaged snacks increase inflammation
Foods That May Help
- Low-fat dairy — skim milk may help reduce uric acid and flare-ups
- Cherries — research shows they can lower uric acid and reduce gout attacks
- Coffee — regular consumption may lower uric acid levels
- Vitamin C-rich foods — citrus, bell peppers, strawberries
- Water — 5-8 glasses daily helps kidneys flush uric acid
- Most vegetables — even higher-purine vegetables don’t seem to trigger gout
The DASH diet and Mediterranean diet are both recommended for gout prevention — they’re rich in vegetables and limit meat consumption.
When to See a Doctor
See a healthcare provider if you experience:
- Sudden, severe joint pain
- Joint pain accompanied by fever
- Multiple gout attacks per year
- Visible lumps under your skin (tophi)
The Bottom Line
Gout is painful but highly treatable. With early diagnosis, proper medication, and lifestyle changes — especially diet modifications — most people can prevent flares and avoid long-term joint damage. If you’ve had a gout attack, work with your doctor to develop a prevention plan that keeps uric acid levels under control.
Sources: NIH MedlinePlus, Cleveland Clinic, CDC, National Kidney Foundation, WebMD